Analgesic Effect of Ethanol Extract of Dillenia ochreata (Miq.) Teijsm. & Binn. Ex Martelli in Wistar Rats
DOI:
https://doi.org/10.22437/chp.v9i1.43080Keywords:
Analgesic , Dillenia ochreata, formalin test, hot plate test, receptorsAbstract
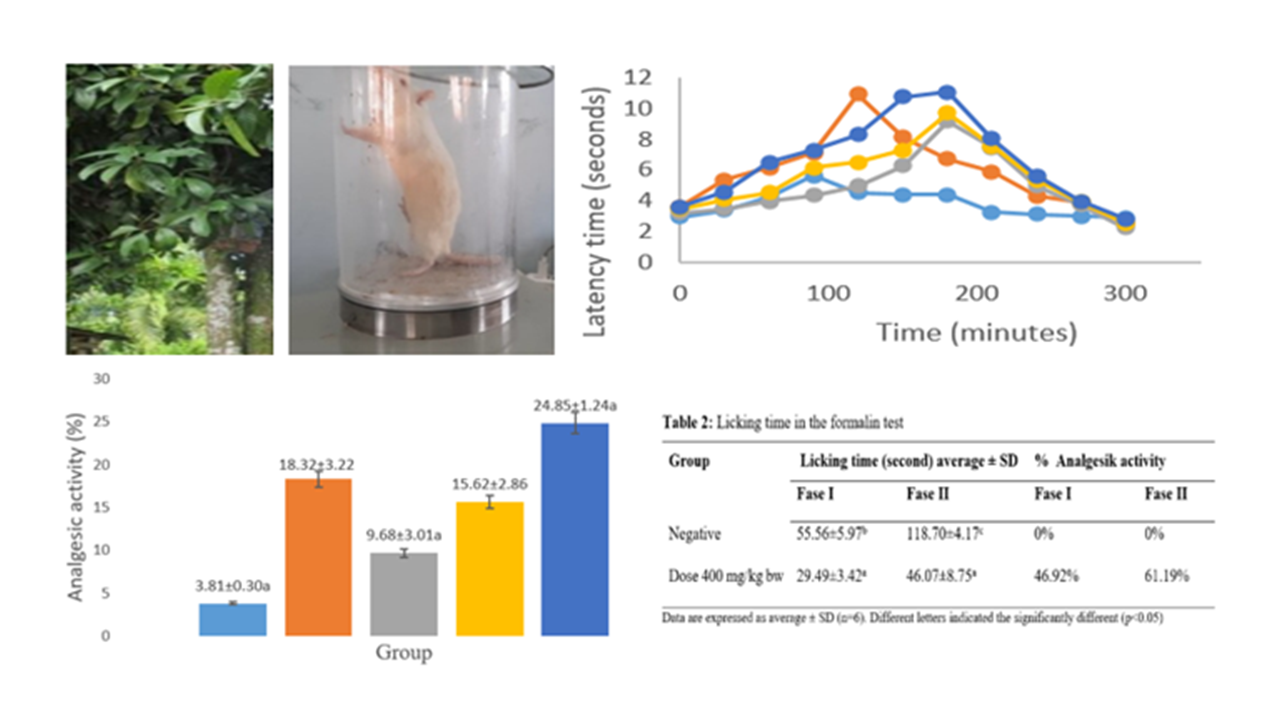
Dillenia ochreata is a traditional medicine used to treat wounds and scabies. In wound healing, one of the treatments is to reduce pain (analgesic). Some compounds of triterpenoid groups have been known to be active as analgesic compounds. The leaf of D. ochrea was reported to contain secondary metabolites triterpenoid centulic acid and 3β-glucopyranosyl-lup-20(29)-en-28 oat. This study aimed to evaluate the analgesic activity and standardization of the ethanol extract of D. ochreata leaf and determine the mechanism of action. Analgesic activity was determined by a hot plate method and formalin test, and the mechanism of action was through muscarinic, dopamine, and opiate receptors, standardization of extract using the method issued by the Indonesian Ministry of Health. The ethanol extract of D. ochreata leaf at a 400 mg/kg bw dose has higher analgesic activity (24.85%) than the positive control (18.32%). Statistical analysis showed a significant difference in analgesic activity percentage between the positive group and those with a 400 mg/kg bw group dose. The 400 mg/kg bw dose also showed a significant difference (p<0.05) between neurogenic pain (46.92%) and inflammation (61.19%) in the formalin test caused by opioid receptors. The evaluation of the analgesic mechanism showed the ethanol extract of D. ochreata leaf works through opioid receptors. The extract meets the requirements of the standard parameters. The leaf extract of D. ochreata can be developed as an anti-analgesic from natural medicine.
Downloads
References
[1] Sohail R, Mathew M, Patel KK, Reddy SA, Haider Z, and Naria M. Effects of Non-steroidal Anti-inflammatory Drugs (NSAIDs) and Gastroprotective NSAIDs on the Gastrointestinal Tract: A Narrative Review”. Cureus. 2023;15(4): 1–14. doi: 10.7759/cureus.37080.
[2] Heyne, K. (1997). Tumbuhan Berguna Indonesia. Jakarta: Yayasan Sarana Wana Jaya.
[3] Muharni M, Amriani A, Fitrya F, Mukafi A. Wound healing activity of Dillenia ochreata leaves ethanol extract in Wistar rats". Journal of Pharmacy &. Pharmacognosy Research. 2022; 10(5) : 896-904. doi: 10.56499/jppres22.1444_10.5.896
[4] Muharni M, Choirunnisa N, and Fitrya F. A Subchronic Toxicity Test of Dillenia ochreata Leaves Extract on Wistar rats". Tropical Journal of Natural Product Research. 2023;7(11), 5244-5249. doi: 10.26538/tjnpr/v7i11.32
[5] Muharni M, Dasuni D, Yohandini H, Ferlinahayati F, Eliza E, and Fitrya F. The antibacterial activity of triterpenoid acid from the ethyl acetate extract of Dillenia ochreata leaves”. Journal of Research in Pharmacy. 2023; 27(6): 2270–2276. doi: 10.29228/jrp.515. [5]
[6] Yohandini H, Muharni M, and Candra PSA. Antibacterial Compound from n-Hexane Fraction of Dillenia ochreata Leaves”. Indonesian Journal of Fundamental and Applied Chemistry. 2023;8(2): 63-69. doi:10.24845/ijfac.v8.i2.63.
[7] Itoh T, Katsurayama K, Efdi M, Ninomiya M, and Koketsu M. Sentulic acid isolated from Sandoricum koetjape Merr attenuates lipopolysaccharide and interferon gamma co-stimulated nitric oxide production in murine macrophage RAW264 cells. Bioorganic & Medicinal Chemistry Letters. 2018;28(22): 3496–3501. doi: 10.1016/j.bmcl.2018.10.008.
[8] Sene M, Ndiaye D, Gassama A, Barboza FS, Mbaye MD, and Yoro SYG. Analgesic and Anti-inflammatory Activities of Triterpenoid Molecules Isolated from the Leaves of Combretum glutinosum Perr. Ex DC (Combretaceae)". Journal of Advances in Medical and Pharmaceutical Sciences. 201819(4): 1-8. doi: 10.9734/JAMPS/2018/v19i430096
[9] Gong JH, Zhang CM, Wu B, Zhang ZX, Zhou, Zhu JH, Liu LH, Rong Y, Yin Q, Chen YT, Zheng R, Yang GZ, Yang XF, and Chen S. Central and peripheral analgesic active components of triterpenoid saponins from Stauntonia chinensis and their action mechanism. Frontiers in Pharmacology. 2023;16;14:1275041. doi: 10.3389/fphar.2023.1275041
[10] Raveendran S, Tilak AV, Yadav A, Das S, Madrewar V, and Kulkarni V. A study to evaluate the analgesic activity of Origanum vulgare in mice using hot plate method”. International Journal of Basic Clinical Pharmacology. 2019;8(7): 1563-1566. doi: 10.18203/2319-2003.ijbcp20192650.
[11] Hijazi MA, El-Mallah A, Aboul-Ela M, and A. Ellakany. Evaluation of Analgesic Activity of Papaver libanoticum Extract in Mice: Involvement of Opioids Receptors”. Evidence-Based Complementary and Alternative Medicine. 2017(1): 8935085. doi: 10.1155/2017/8935085.
[12] Shojaii A, Motaghinejad M, Norouzi S, and Motevalian A. Evaluation of Anti-inflammatory and Analgesic Activity of the Extract and Fractions of Astragalus hamosus in Animal Models. Iranian Journal of Pharmaceutical Research.2015;14(1). 263–269.
[13] Alam MB, Rahman MS, Hasan M, Khan MM, Nahar K, and Sultana S. Antinociceptive and Antioxidant Activities of the Dillenia indica Bark,” International Journal of Pharmacology. 2012;8(4): 243–251. doi: 10.3923/ijp.2012.243.251.
[14] Kementerian Kesehatan RI. (2017). "Farmakope Herbal Indonesia". 2nd ed. Jakarta: Direktorat Jenderal Kefarmasian dan Alat Kesehatan. [14]
[15] Thenarasu V, Gurunathan D, and Santhosh MP, Kumar. Comparison of Efficacy of Diclofenac and Paracetamol as Preemptive Analgesic Agent. Biomedical and . Pharmacology Journal. 2018;11(3): 1699–1706. doi: 10.13005/bpj/1539.
[16] Hoy SM. Diclofenac Sodium Bolus Injection (DylojectTM): A Review in Acute Pain Management”. Drugs. 2016;76(12): 1213–1220. doi: 10.1007/s40265-016-0619-7.
[17] Jepma M, Jones M, and Wager TD. The dynamics of pain: Evidence for Simultaneous Site-Specific Habituation and Site-Nonspecific Sensitization in Thermal Pain. The Journal of Pain.2014;15(7): 734–746. doi: 10.1016/j.jpain.2014.02.010.
[18] McPherson C, Miller SP, El-Dib M, Massaro AN, and Inde TE. The influence of pain, agitation, and their management on the immature brain”. Pediatric Research. 2020;88:168–175. doi: 10.1038/s41390-019-0744-6
[19] Singh PA, Brindavanam NA, Kimothi GP, Aeri V. Evaluation of in vivo anti-inflammatory and analgesic activity of Dillenia indica f. elongata (Miq.) Miq. and Shorea robusta stem bark extracts. Asian Pacific Journal of Tropical Disease.2016;6(1): 75 -81. doi:10.1016/S2222-1808(15)60988-4
[20] Jalil J, Sabandar CW, Ahmat N, Jamal JA, Jantan I, Aladdin NA, and Sahidin I. Inhibitory Effect of Triterpenoids from Dillenia serrata (Dilleniaceae) on Prostaglandin E2 Production and Quantitative HPLC Analysis of Its Koetjapic Acid and Betulinic Acid Contents”. Molecules. 2015;20(2): 3206–3220. doi: 10.3390/molecules20023206.
[21] Ortiz-Placín C, Castillejo-Rufo A, Estarás M, and González A. Membrane Lipid Derivatives: Roles of Arachidonic Acid and Its Metabolites in Pancreatic Physiology and Pathophysiology. Molecules. 2023; 28(11): 4316. doi: 10.3390/molecules28114316.
[22] B. Wang, L. Wu, J. Chen, L. Dong, C. Chen, Z. Wen, J. Hu, I. Fleming and D We. (2021). “Metabolism pathways of arachidonic acids: mechanisms and potential therapeutic targets,” Signal Transduction and Targeted Therapy. 6(94): 1-30. doi: 10.1038/s41392-020-00443-w.
[23] Chang HY, Sheu MJ, Yang CH, Lu TC, Chang YS, Peng WH, Huang SS, Huang GJ. Analgesic effects and the mechanisms of anti-inflammation of hispolon in mice. Evid Based Complement Alternat Med. 2011;2011:478246. doi: 10.1093/ecam/nep027
[24] Khatri R, Ahmad M, Pal G, and Ashwlayan V. Evaluation of antinociceptive activity of Ajuga bracteosa wall ex benth”. International Journal of Green Pharmacy. 2013; 7(1): 73-76. doi: 10.4103/0973-8258.111631.
[25] Deraniyagala SA, Ratnasooriya WD, and Wijesekara PS. Antinociceptive activity of aqueous fruit extract of Dillenia retusa T. in rats”. International Journal of Advances in Pharmacy, Biology, and Chemistry.2014; 3(2): 371–377.
[26] Dalefield ML, Scouller B, Bibi R, and Kivell BM. The Kappa Opioid Receptor: A Promising Therapeutic Target for Multiple Pathologies”. Frontiers in Pharmacology. 2022;13(837671):1–26. doi: 10.3389/fphar.2022.837671.
[27] Mas-Orea X, Basso L, Blanpied C, Gaveriaux-Ruff C, Cenac N, and Dietrich G. Delta opioid receptors on nociceptive sensory neurons mediate peripheral endogenous analgesia in colitis”. Journal of Neuroinflammation. 2022;19(1): 1-7. doi: 10.1186/s12974-021-02352-3.
[28] Heyns, I. M., Faunce, A. F., Mumba, M. N., Kumar, M. N. V. R., & Arora, M. Nanotechnology-Enhanced Naloxone and Alternative Treatments for Opioid Addiction. ACS pharmacology & translational science, 2024; 7(8), 2237–2250. https://doi.org/10.1021/acsptsci.4c00158
[29] Maia JL, Lima-Júnior RCP, David JP, David J M, Santos FA, and Rao VS. Oleanolic Acid, a Pentacyclic Triterpene Attenuates the Mustard Oil-Induced Colonic Nociception in Mice. Biological & Pharmaceutical Bulletin. 2006; 29(1): 82–85. doi: 10.1248/bpb.29.82.
[30] Gundamraj S and Hasbun R. The Use of Adjunctive Steroids in Central Nervous Infections. Frontiers in Cellular and Infection Microbiology. 2020; 10(592017): 1–13. doi: 10.3389/fcimb.2020.592017.
[31] Higginbotham JA, Markovic T, Massaly N, and Morón JA. Endogenous opioid systems alterations in pain and opioid use disorder. Frontier in Systeam Neuroscience. 2022; 16(014768): 1–24. doi: 10.3389/fnsys.2022.1014768.
[32] Purnomo Y and Tilaqza A. Analgesic and Anti-inflammatory Activities of Urena lobata L. Leaf Extracts. Indonesian Journal of Pharmacy.2022;33(4): 566–574, doi: 10.22146/ijp.2145.
[33] Sullivan LC, Chavera TA, Gao X, Pando MM, and Berg KA. Regulation of δ Opioid Receptor-Mediated Signaling and Antinociception in Peripheral Sensory Neurons by Arachidonic Acid–Dependent 12/15-Lipoxygenase Metabolites. The Journal of Pharmacology and Experimental Therapeutics. 2017;362(1): 200–209, Jul. doi: 10.1124/jpet.117.241604.
[34] Syukri Y, Purwati R, Hazami N, Tahmid HA, and Fitria A. Standardization of Specific and Non-Specific Parameters of Propolis Extract as Raw Material for Herbal Product”. EKSAKTA: Journal of Sciences and Data Analysis. 2020;1(1): 36–43. doi: 10.20885/EKSAKTA.vol1.iss1.art6.
Published
Versions
- 2026-01-20 (2)
- 2025-06-30 (1)